Ann Arbor
Ann Arbor PDCEN

The VA Ann Arbor Medical Center is committed to improving the care of Veterans with concerns about their post-deployment respiratory health. To accomplish this objective, we are active in the realms of clinical care, education, and research. From a clinical perspective, our PDCEN evaluations provide Veteran-centered, state-of-the-art clinical care using a multi-disciplinary approach that incorporates specialists in Pulmonary, Environmental, and Sleep Medicine. Assisted by PDCEN funding, we have increased our testing capabilities to include Forced Oscillometry and Exhaled Nitric Oxide assessments. To improve Veteran's access to this specialty care within our VISN, we have opened a Post-Deployment Respiratory Health Clinic which will help us identify Veterans appropriate for a full PDCEN evaluation and provide opportunities for Veterans to receive local follow-up care once the initial evaluation is complete. Hear more about our mission and function from our site director, Dr. John Osterholzer, by watching the video below.
To improve awareness about deployment related respiratory disease, we published an article in the New England Journal of Medicine's Clinical Problem Solving series describing the presentation of a Veteran diagnosed with constrictive bronchiolitis and highlighting the Airborne Hazards and Open Burn Pit Center of Excellence's role in establishing the diagnosis (https://pubmed.ncbi.nlm.nih.gov/35388671/).
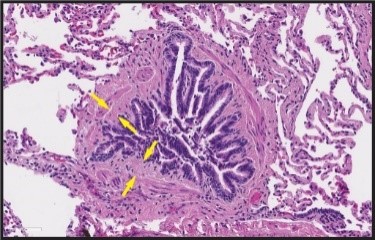
Figure 2. Biopsy Specimen of the Right Lung.
Hematoxylin and eosin stained section of lung demonstrates constrictive bronchiolitis (CB) characterized by subepithelial fibrosis that widens (arrows) the normally narrow space between the airway epithelium and smooth muscle (200x magnification). Rabin et al; N Engl J Med. 2022
Our Post-Deployment Respiratory Health Research Program is actively pursuing both basic science and clinical research projects. Our basic science research group developed and described a novel animal model of constrictive bronchiolitis (CB) in mice that displays features of airway abnormalities comparable to what is observed in Veterans with deployment related constrictive bronchiolitis. This study expands our understanding of how airborne hazards may injury the airway epithelium leading to small airway inflammation and fibrosis (https://pubmed.ncbi.nlm.nih.gov/34954211/).
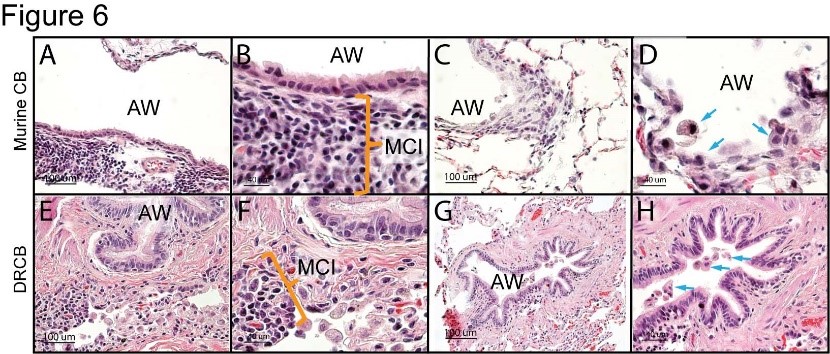
Figure 6. Chronic airway inflammation in murine and deployment-related CB. (A-H) Representative images of lung sections (H & E stained) obtained from a CC-DTA mouse (A – D) at protocol d20, and a veteran diagnosed with DRCB (E – H). Note the peribronchiolar mononuclear cell infiltrates (orange braces in B, F) and collections of intraluminal cells with the appearance of foamy macrophages (blue arrows in D, H) present in both specimens. AW; airway. MCI; mononuclear cell infiltrates. Scale bars 100μm (A, C, E, G) and 40μm (B, D, F, H). Teitz-Tennenbaum et al; Am J Pathol. 2022
In partnership with the Department of Radiology at the University of Michigan, our clinical research group published a study demonstrating that the amount of functional small airways disease identified using quantitative CT scan analysis performed on CT scans obtained from military personnel diagnosed with constrictive bronchiolitis is increased relative to healthy subjects and greater than subjects with moderate chronic obstructive pulmonary disease (https://pubmed.ncbi.nlm.nih.gov/35608541/).
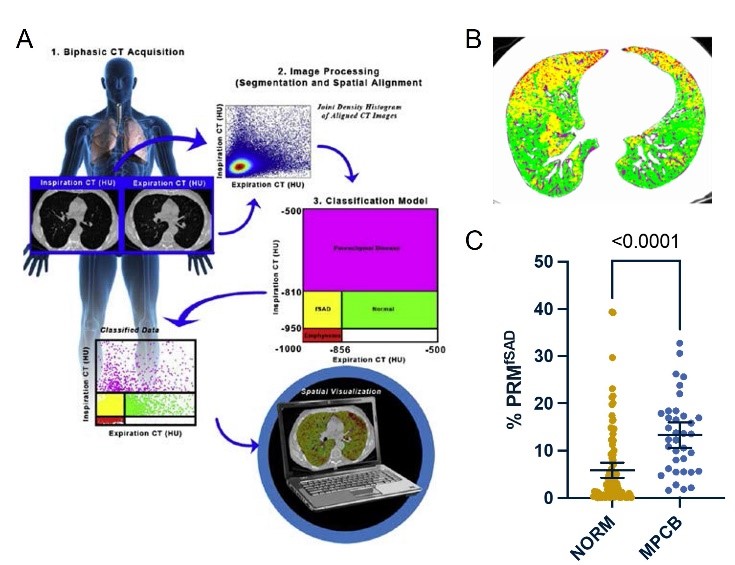
(A) Quantitative CT analysis using parametric response mapping identifies and quantifies different lung abnormalities including functional small airways disease (fSAD). (B) Increased fSAD (yellow) identified in the CT scan images obtained from a Veteran diagnosed with constrictive bronchiolitis. (C) Unadjusted analysis showing that the percent of fSAD in military personnel with constrictive bronchiolitis (MPCB) is increased 2-fold relative to healthy control subjects (NORM). Davis, et al; Am J Respir Crit Care Med. 2022
We hope this finding will lead to improvements in the diagnosis of deployment-related respiratory disease amongst Veterans and believe these results help explain the degree of symptoms that they experience.
To promote awareness of the Sergeant First Class Heath Robinson Honoring our Promise to Address Comprehensive Toxics (PACT) Act, we recently published a Perspective in the Annals of the American Thoracic Society entitled "A Sacred Obligation: Meeting the Needs of Veterans with Airborne Hazard Exposures."



















